Androgenetic Alopecia
What is Androgenetic Alopecia
Androgenetic alopecia is the most common form of hair loss worldwide, affecting both men and women. Often referred to as “male-pattern baldness” or “female-pattern hair loss,” it is a genetically influenced condition that causes gradual thinning and shrinkage of the hair follicles. This condition develops when follicles become sensitive to androgens—particularly dihydrotestosterone (DHT)—which progressively shortens the anagen (growth) phase of the hair cycle. Over time, affected follicles produce finer, shorter, and weaker strands, eventually becoming unable to produce visible hair.
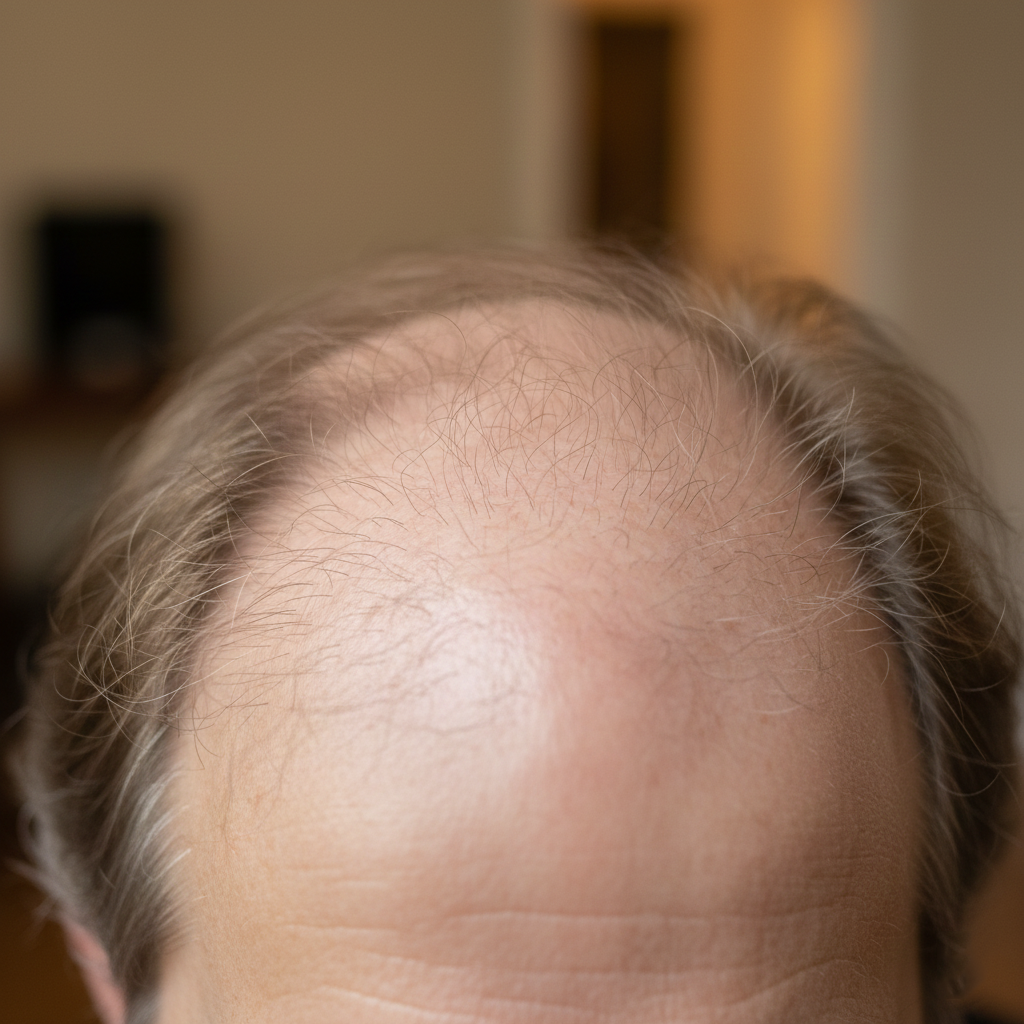
In men, androgenetic alopecia typically appears as a receding hairline, thinning at the temples, and gradual loss at the crown. Recognizing these early signs can empower individuals to seek treatment promptly, helping slow progression and maintain scalp health, fostering a sense of hope and control.
What Are the Causes
The combination of genetics and hormonal sensitivity explains the condition, helping the audience feel more informed and less uncertain about its causes.
Genetic inheritance plays a significant role. Individuals with a family history of pattern hair loss—whether maternal or paternal—have a higher likelihood of developing the condition themselves. Hormonal fluctuations can also influence progression. Men with naturally higher androgen levels may experience an earlier onset, while women may notice worsening during perimenopause and menopause due to declining estrogen levels. Recognizing these factors can help readers understand their personal risk and the importance of monitoring hormonal health.
Other contributing factors may include chronic stress, nutritional deficiencies, scalp inflammation, and environmental factors that affect hormonal balance. Although these do not directly cause androgenetic alopecia, they may accelerate shedding or worsen thinning when combined with genetic predisposition. Because this condition is hormonally and genetically driven, it behaves differently from other types of alopecia and requires an accurate understanding of its root mechanisms.
Symptoms
In men, early signs include a receding hairline or thinning at the temples, with progressive loss at the crown, often feeling finer or weaker long before bald spots appear, helping readers identify early symptoms.
Women typically do not experience frontal recession. Instead, they may notice diffuse thinning across the central scalp, decreased volume, difficulty achieving fullness, or a wider part line. The frontal hairline generally remains intact, but density decreases along the top and crown. Women may also experience greater shedding during hormonal transitions such as postpartum or menopause.
In all individuals, the hallmark symptom is follicular miniaturization—producing thin, wispy strands that lack strength. Excessive shedding may be present in the early stages, especially during telogen effluvium episodes, which can overlap with pattern thinning. The scalp may become more visible under bright lights or when the hair is wet. Because the progression is slow and steady, many individuals do not recognize changes until significant density has been lost.
How Many People Are Affected
Androgenetic alopecia progresses gradually, and symptoms often begin subtly. In men, early signs may include a receding hairline or thinning around the temples, followed by progressive loss at the crown. Over time, these areas may expand and eventually connect, forming the classic “M-shaped” pattern. Hair may feel finer, weaker, or less voluminous long before visible bald spots appear.
Women typically do not experience frontal recession. Instead, they may notice diffuse thinning across the central scalp, decreased volume, difficulty achieving fullness, or a wider part line. The frontal hairline generally remains intact, but density decreases along the top and crown. Women may also experience greater shedding during hormonal transitions such as postpartum or menopause.
In all individuals, the hallmark symptom is follicular miniaturization—producing thin, wispy strands that lack strength. Excessive shedding may be present in the early stages, especially during telogen effluvium episodes, which can overlap with pattern thinning. The scalp may become more visible under bright lights or when the hair is wet. Because the progression is slow and steady, many individuals do not recognize changes until significant density has been lost.
Complications
While not physically harmful, androgenetic alopecia can affect emotional well-being, making individuals feel understood, supported, and less alone in their experience.
If left unmanaged, long-standing androgenetic alopecia may lead to extensive follicle miniaturization. Over time, follicles can become dormant or replaced by fibrotic tissue, reducing the potential for natural regrowth. This is especially true for individuals who experience early-onset or rapid progression.
Scalp visibility may increase, especially under bright light or with certain hairstyles. Thinning hair can become more brittle and break easily, leading to uneven textures or a loss of volume. The emotional burden associated with long-term thinning often affects social interactions and self-esteem. Early awareness and accurate diagnosis are essential to prevent further progression.
Diagnosis
Diagnosing androgenetic alopecia early is essential because it allows for timely intervention, which can slow progression and improve treatment success, helping individuals feel hopeful and empowered to take action.
Dermoscopy or trichoscopy provides magnified visualization of the follicles, allowing clinicians to observe variation in hair shaft diameter—a hallmark of androgenetic alopecia. This tool helps distinguish the condition from telogen effluvium or autoimmune causes such as alopecia areata.
Blood tests may be recommended to rule out thyroid disorders, iron deficiency, hormonal imbalances, vitamin D deficiency, or autoimmune markers. While these do not cause androgenetic alopecia, they can influence shedding and worsen thinning if present. In rare cases, a scalp biopsy may be performed to confirm the diagnosis or rule out scarring alopecia. Accurate diagnosis ensures that patients understand the progressive nature of this condition and can pursue appropriate management strategies. Early diagnosis is crucial to prevent further hair loss and improve treatment outcomes.
Treatment Options
Treatment options for androgenetic alopecia focus on protecting existing follicles, slowing further thinning, and supporting overall scalp health. Lifestyle adjustments, such as reducing high-stress habits, optimizing nutrition, and avoiding excessive heat or chemical treatments, can help minimize further damage. Scalp care that includes gentle cleansing, improved circulation, and reduced inflammation supports a healthier environment for hair growth.
Medical therapies may be recommended to stabilize shedding or support follicle function. In individuals with hormonal influences—particularly women experiencing menopausal changes—addressing underlying hormonal imbalances may help improve hair density. Anti-inflammatory treatment may be beneficial for those with scalp irritation or chronic flaking conditions that coexist with androgenetic alopecia.
In many instances, procedural interventions or regenerative options may help support function and repair, such as PRP, Exosomes, Stem Cells, LLLT, Peptides, Microneedling, Diagnostic Ultrasound, and Shockwave.
In cases with advanced thinning, non-surgical aesthetic approaches or restorative techniques may be considered to improve visual density. Early intervention is crucial, as follicles affected for extended periods may lose their ability to produce new hair.
